Welcome to On The Mind, a collection of stories, news, and analyses on the startups, investors, and thought leaders in mental health and wellness.
Here’s what’s included in issue No. 6:
A Stanford-founded precision mental health startup utilizing genetic testing
A brief overview of twin studies and the future of psychiatric genetics
Applying the Stockdale Paradox as a mindfulness practice
🎙️ Interview with Maurice Chiang, CEO of Prairie Health
Conversations with founders, investors, and thought leaders in mental health and wellness.
At Prairie Health, every member gets a genetic test when they’re first onboarded. Unlike companies such as 23andMe and Ancestry, the genetic test results themselves aren’t the product. Instead, Prairie draws insights from your test and pairs you with a mental health provider who considers your genetic profile in developing a treatment plan.
Prairie connects members with psychiatrists and care partners to provide ongoing support. If medications are deemed a relevant part of the treatment plan, that’s something Prairie also facilitates through discreet delivery.
This week I spoke with Prairie’s CEO, Maurice Chiang, about his vision for applying precision medicine to psychiatry. He co-founded the company with three of his Stanford classmates, Benson Kung (heads research & development), Aaron Kappe (leads business strategy and growth), and Jin Woo Yu (heads product and engineering).
Below I dive into the team’s efforts to change the way we deliver mental healthcare, from improving access to following through on higher quality care.
Why did you decide to start Prarie?
Our team was all aligned on the challenges that we saw plauging mental health. We saw how hard it is to get in the door. We saw how, once you’re actually getting treated, the first line of therapy is so often just a trial-and-error method to test what works. And we saw how the mental health system was not designed for the people who use it or need it the most - it’s traditionally been some white guy giving you a choice between a few antidepressants, many of which were only studied on other white guys before the NIH mandated that minorities and women be included in clinical research.
From our own experience we know how challenging finding the right medication can be, and how disconnected the whole care process is - trying a random medication, experiencing terrible side effects, nobody following-up with you. We believe that we can and should do better. The future of psychiatry will be more data-driven, and we started Prairie to help lead that.
And what’s up with the name Prairie Health?
The reason behind the name is actually two-fold.
First off, a prairie is just this pastoral, peaceful place away from technology, away from the city, away from the stresses of daily life. So it captures that peaceful feeling people associate with a prairie.
Second is the prairie vole. It’s one of the canonical examples used in behavioral biology to talk about pair bonding. They’re a pair bonding animal - when they meet, they stick together for life. That’s the kind of ethos we want to share with our members. We’re really here to support you from finding the right medication, to checking up with you while you’re undergoing treatment, seeing if your symptoms are okay and if you’re able to manage any side effects. We’re a shoulder to lean on through the care process.
How have you approached designing Prairie?
It’s been a long, long journey. We started with a traditional design thinking approach - in product creation, you want to focus on what needs the MVP is solving for, without allowing for scope creep.
In healthcare, it’s particularly hard to avoid that scope creep because you’re designing products around so many stakeholders. It’s more than just improving care. You need buy-in from payers, who need data and actuarial outcomes and ROI in order to reimburse the solutions. Providers are busy enough as it is, and especially at the primary care level the last thing they want is another tool integrating into their EHR and slowing down their workflow.
Then there’s the question of how you design the business model. We thought about how it might make sense to work with self-insured employers, having Prairie reimbursed for employees. There’s a valuable market there, but there are incentive misalignment issues that dissuaded us. The stakeholder making the decision on behalf of employers is the benefits manager, who often just wants to check the box of providing a cost effective solution to their employee population. They’re not thinking about the unintuitive logic of bringing on more expensive services for employees with clinical anxiety and depression in order to drive better outcomes that ultimately lower their downstream medical costs.
Instead, we landed with a DTC approach, where the value is most aligned. Patients care about getting treatment that works for their bodies, and providers are bought in because they’re getting paid for their services. The DTC space is a testing ground for us, allowing us to collect real world data on patient outcomes, engagement, satisfaction, and retention, setting us up for a longer-term approach where we can eventually work with payers to demonstrate how we can improve their bottom line.
One of your big differentiators is the genetic testing component. What does a person’s genetic test tell you about their mental health?
Taking a step back, we think there are a lot of different data streams that are important in making better clinical decisions in mental healthcare. Genetic testing is just one of those inputs.
It’s important to understand what the evidence base of genetic testing says today. It’s not true to say a genetic test can tell you which medication to take and at what dosage. That’s not what we claim.
Ultimately, genetic testing does inform our treatment plans and helps reduce negative side effects. We look at biomarkers and metabolism to identify when someone might be better suited for a lower starting dosage, or whether a specific medication may not metabolize well in a patient’s body. Genetic testing is not a very expensive thing to do and provides another data point to guide higher quality care.
On the medication selection side, our research work plays a larger role. Our researchers work with machine learning and natural language processing techniques to sort through free text data and go through clinical directories to get a better sense for patient subtypes. Based on the past 20 years of clinical free text data, we can segment out a cohort of people who look genetically similar to you and evaluate how they responded to specific treatments. We can then apply probabilistic medicine to decide which medications to start people on and use genetic testing to inform the dosage. For example, a 90-pound Hispanic female shouldn’t have the same medication protocol as a 200-pound white male.
How do you see care teams evolving in a future where you can just get a bunch of data scientists to crunch the numbers and determine the best treatment plan?
At Prairie we have a very technical team for what we think is a very technical problem. All of us come from STEM backgrounds.
We definitely believe data science plays a role in the future of medicine. That being said, it’s a common trope in Silicon Valley to say that we can use technology to solve anything. We don’t believe that.
We think psychiatrists are the most informed about mental health today and should be at the helm of clinical decisions. We view data science as a pillar that can enable psychiatrists to provide better care, not as something that will replace them.
Part of the Prairie model includes the option for medication delivery. There’s been some criticism of mental health startups that push subscription antidepressants on patients. Is this something you’re concerned about?
Part of our core ethos, our North Star, is a focus on outcomes.
There are definitely a lot of DTC companies out there today who aren’t doing patients a service. Sure, the DTC model improves access to care at a lower price, but the last thing we need is a technology-enabled pill pusher in psychiatry. We use a DTC approach as a means of collecting data on outcomes that can help us expand to a sustainable model of managed care.
Our stance at Prairie is that there are a lot of people who have mental illnesses who need better care. Some just need therapy, and when medication is not the right choice for people, we certainly respect that. There is a good contingent of people who do need medication, and medication is proven to help, especially alongside therapy. Our model is focused on getting people the right medication the first time, getting them properly medicated, and getting them off, if and when it’s no longer needed. For us, patient outcomes always comes first, which is why we’ve doubled down on genetic testing, care management, research and development, and our machine learning platform.
Let’s talk about your fundraising journey. What’s been your experience?
We’re venture-backed, but have been pretty quiet about it. We last raised in the first half of 2020, and are back at it with our current round now. We’ve had five institutional investors on board since last year, and given that we view this round as one in the same as our last raise, we want to give current investors the optionality to continue to invest in what we’re doing given our progress.
Better Ventures was one of the bigger players in our last round. They’ve been fantastic and are very mission-aligned.
We’re always looking for value-add investors that can help us accelerate our growth. To us, that’s folks with expertise in healthcare and DTC (especially as it relates to healthcare products), those who can help with hiring and strategic direction around ML/AI and genetics, and those with a data-driven focus. We value connections to industry partners as we continue to grow.
A lot of what you’re building feels like the next step in precision mental health. How do you see the space changing over the next 5-10 years?
Mental health in general has so much innovation going on today.
In the venture community of course, psychedelics are of interest. We’ll see more innovative therapeutic options available for patients in the next decade, with treatment modalities that extend beyond SSRIs.
More broadly, we see a trend of more data-driven care. In 5-10 years, when a patient enters the doctor’s office or Zoom waiting room, they’ll expect their data is being used to inform their treatment. Genetic testing and biomarkers will be used, supported by longitudinal data collected between visits and the application of machine learning to large phenotypic data sets of populations. I expect a multitude of better ways to measure outcomes and make care decisions.
The general attention on mental health will continue to grow. It’s a dream of mine that people really start to treat mental illness in the same way they treat physical illness. It’s reimbursed at the same rates, or maybe there’s even a world where insurance doesn’t exist. Access to care is on parity with physical health. Conversations in the workfroce are destigmitized and encouraged.
There’s a bright future ahead.
You hit on a lot of what excites me in the space. Last question - for those who want to create a world that’s a bit more like a prairie - are you hiring?
We are! We’re looking for care managers, typically MSWs who have professional mental health backgrounds and who can help with care coordination and checking in on our members.
We’re also contracting psychiatrists.
On the product side, we’re looking for software engineers.
🩺 Clinical Coverage
Discussion of clinical concepts, studies, or perspectives on mental health and wellbeing.
It’s only natural that I focus on genetics for this week’s clinical coverage. As mentioned, Prairie uses genetic testing as one of many inputs to help inform a patient’s treatment protocol. We’re still in the early innings of understanding the brain and mental disorders through the lens of genetics.
Research has shown, however, that there is a strong hereditary component to mental illness. Familial risk has been documented through twin studies, where the prevalence of certain mental disorders has been tracked for identical twins (who share 100% of their genes) and fraternal twins (who share 50% of their genes). For example, if one identical twin has bipolar disorder, there is a 60-80% chance the other twin also has the disorder. If one fraternal twin has bipolar disorder, there is only an 8% chance the other twin has it.
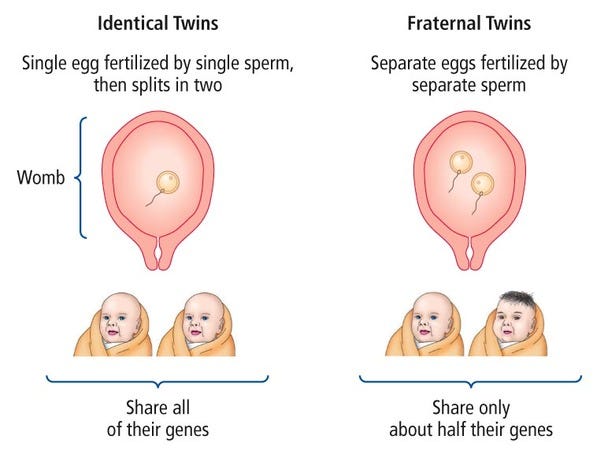
According to the National Institute of Mental Health's Genetics Workgroup, despite the strong evidence that genetics play a significant role in susceptibility to mental health disorders, no specific gene has been identified for common mental disorders. It’s expected that this is due to the strong role environmental factors also play in modulating the genetic susceptibility to mental disorders.
There’s a ton to uncover at the intersection of psychiatry and genetics. The Genetics Workgroup mentioned above released a detailed report of recommendations on how to advance research, which hints at some of the opportunities and challenges that lie ahead.
💰 Recent Investments and IPOs
Rundown of recent investment news in mental health and wellness companies.
actio, the German-based live coaching app, extended its Seed round to ~$12.2M with new investor Heal Capital (Link)
Alleva, which makes software for the behavioral health industry, raised an undisclosed amount in its Seed round (Link)
Beam, a CBD and wellness brand, raised a $5M Series A led by C2 Ventures (Link)
Chorus, a meditation app with a social layer, received funding as part of Y Combinator’s Winter 2021 batch of startups (Link)
Eden Health, the concierge healthcare provider that incorporates behavioral health services, raised $60M in its Series C led by Insight Partners (Link)
Equip, a virtual eating disorder treatment program, raised $13M in a Series A round led by Optum Ventures, with participation from .406 Ventures and F-Prime Capital (Link)
Flow Neuroscience has purchased Halo Neuroscience for an undisclosed sum. Both companies focus on brain stimulation technology to improve health outcomes (Link)
HearMe, a Poland-based company providing employee mental health services, raised a Pre-Seed round of ~$120,000 led by Think Bigger Capital (Link)
Innerjoy, an Istanbul-based personalized meditation app, raised an undisclosed sum in its Seed round (Link)
Koa Health, a digital mental healthcare provider, closed an oversubscribed $36M Series A round led by Wellington Partners Life Sciences and Ancora Finance Group. The round had an initial close back in October 2020 (Link)
Maya, a startup focused on accessible healthcare in Asia, especially for sensitive issues including mental health, raised a $2.2M Seed led by Anchorless Bangladesh and The Osiris Group (Link)
Mainstay Medical, a developer of neurostimulation technology that targets chronic pain, raised $108M in a round co-led by Ally Bridge Group and Sofinnova Partners (Link)
Modern Health, the mental health platform for employers, raised $74M in a Series D round that pushes its valuation to unicorn status at $1.17B. The round was led by Founders Fund with support from existing investors Battery Ventures, Kleiner Perkins Caufield & Byers, and Felicis Ventures (Link)
People Matter, maker of the app Okina touted as a “Fitbit for mental health,” raised ~$700,000 (Link)
Pipeline Therapeutics, a biopharmaceutical company focused on the development and commercialization of first-in-class small molecules for neuroregeneration, raised an $80M Series C (Link)
Talkiatry, a telepsychiatry startup, raised a $5M Series A led by Sikwoo Capital Partners (Link)
Quilt, an audio-based social network focused on self-care, raised a $3.5M Seed round led by Mayfield Fund (Link)
📖 Interesting Reads
Sometimes mental health-related. Sometimes just things I find interesting.
This one is for all of my ‘Flat Earther’ readers (Link)
An eerie look at data collection during the Capitol riots (Link)
Explore this database to find the right mental health app for you (Link)
Benedict Evans provides his annual review, and it doesn’t disappoint (Link)
The growing opportunity for products that enable communities (Link)
HBR covers the impact of Covid-19 on our well-being, in charts (Link)
I think I want to be a pilot now (Link)
Rewinding the internet by 10 years… (Link)
Explore the world, through radio (Link)
Just for a moment, pretend you’re at your favorite bar in a post-Coronavirus world (Link)
Scientists discovered the world’s oldest DNA, from 1.2M years ago (Link)
Perseverance landed on Mars, ICYMI (Link)
Princeton launches “The Manic Monologues” to spotlight mental health (Link)
Pete Wells adapts to New York restaurant reviews during the pandemic (Link)
Thoughts on how the internet is becoming more spontaneous (Link)
🧠 Mindfulness Tip of the Week
Tips to improve your mental health and wellbeing.
I came across a concept that pretty elegantly captures a method of thinking I’ve found myself using at a variety of different points in life, without having a name for it until now. It’s called the Stockdale Paradox.
Admiral James Stockdale was a prisoner of war in Vietnam for nearly 8 years. The paradox he’s now famous for stems from the idea that you can both have faith and confront reality in parallel, even when that reality is dark.
I think the point best sinks in with a couple of direct quotes from Stockdale himself:
“You must never confuse faith that you will prevail in the end—which you can never afford to lose—with the discipline to confront the most brutal facts of your current reality, whatever they might be.”
“I never lost faith in the end of the story. I never doubted not only that I would get out, but also that I would prevail in the end and turn the experience into the defining event of my life, which, in retrospect, I would not trade.”

So what does this all have to do with mindfulness?
You might feel your troubles can’t compare to being a prisoner of war, but there’s really no point in comparison at all. By definition, we’ll each at some point go through the hardest emotional or mental experience within the context of our own lives. Maybe you already have, or maybe the worst-to-date is even in-progress. The Stockdale Paradox is a way of framing your outlook to accept reality, whatever that may be for you, and still maintain optimism.
The pandemic is a great use case for deploying this mindset. It played a role in how I managed my own mental health while living alone in NYC for 2 months during the city’s initial lockdown. And that doesn’t mean I was filled to the brim with happiness during that period - it was isolating, lonely, and anxiety-inducing at times - but I knew it would end, and that enabled me to keep pushing through.
On Your Mind
I’d love your feedback - feel free to email me at tarockoff@berkeley.edu.
If you’re working on something in mental health and wellness, let’s talk. You can book some time with me here.
Know someone who’d enjoy On The Mind?
Was this newsletter forwarded to you?
Written by Daniel Tarockoff, an MBA student at UC Berkeley and former healthcare strategy consultant exploring the future of mental health. Born in Michigan. Based in Berkeley, CA.









