Welcome to On The Mind, a collection of stories, news, and analyses on the startups, investors, and thought leaders in mental health and wellness.
Here’s what’s included in issue No. 9:
Making it easier for providers to deliver mental healthcare
Psilocybin goes head-to-head with a leading SSRI
Applying the Pomodoro Technique to improve your workflow
🎙️ Interview with Dr. Harry Ritter, Founder and CEO of Alma
Conversations with founders, investors, and thought leaders in mental health and wellness.
Harry Ritter grew up in a family that was very passionate about healthcare. Both of his parents were doctors, so he was subject to that life path from a young age, ingraining an appreciation for what it means to commit your life to help others live happier and healthier. It’s why he started down that path himself - but ultimately, after completing medical school and his first year of residency, he stopped practicing in search of a role that better fit his interests within the healthcare field. What followed was a journey through strategy consulting and startups, until 2017 when he founded Alma, a company making it easier for consumers to access high-quality, affordable mental health care by supporting providers in building thriving private practices. I spoke with Harry about how he found his way to behavioral health, Alma’s product offerings, his relationship with investors, and where he sees the industry going.
What made you decide to leave your residency at Mass General?
I’ve always loved medicine and loved healthcare, but I felt like I hadn’t found what I wanted to do clinically. I had started two companies in the past - a college blogging platform as an undergraduate, and a social network for medical students while in medical school. Both were utter flops, but they got me hooked into the business world.
When I started my residency, I was working under Hasan Bazari, this legendary doctor who never said much but was kind of like Yoda, full of wisdom. I remember him emphasizing that we’re in the business of building leaders in healthcare, whatever that looks like. I was motivated to find a role that matched the impact I wanted to make - I ended up applying for a bunch of jobs and landed at McKinsey. I spent a year there, and then made my way to the Oscar Insurance team - I knew a couple of the founding members and really fell in love with the team.
You spent 4 years at Oscar before founding Alma. How did your time at Oscar mold your interest in mental health and your vision for Alma?
At Oscar, behavioral health was so on the side, so undertreated. Across the healthcare field people talked about diabetes, but there wasn’t much conversation around anxiety, which is far more widespread. The majority of people who need care aren’t getting it, and it was obvious this was the biggest opportunity in healthcare today.
Simultaneously, I was managing my dad’s health as a solo caregiver, and started to see a therapist during that experience to deal with the anxiety, grief, and fear. I became a real believer in mental healthcare - and this was after completing my primary care training, where we really hadn’t learned much about behavioral health.
One of the key insights I had watching the rise of mental healthcare was that there was increasing demand alongside an entirely fragmented community of providers. In behavioral health you have mainly single shingle, solo practioners, and I wanted to figure out how to help these providers do better.
My time at Oscar prepared me greatly for creating Alma. For one, it was a really privileged spot to see the needs in the industry. Something that makes Alma unique is how much we work with insurance companies to make sure our members are covered, and everything I’ve applied with our current payer partners comes from my Oscar experience. Secondly, Oscar taught me the value in building a simple product experience. Oscar was great because of its simplicity - there was a flow for how you signed up that was so clean and easy to use. It never cheapened healthcare and made it feel like a game or widget, it was serious, and I retained that orientation of how to build a great product. Finally, I think Oscar is really what instilled the motivation in me to build something big in healthcare. Being in the mix of the disruption that Oscar led got me excited to do the same with Alma.
Where’d the name Alma come from?
We spent some time trying to come up with a name. Alma means “the world” in Aramaic, and “soulfulness” in Latin. We thought, how can you create a business around building soulfulness into the world?
And what does Alma do exactly? What’s the product?
Alma is a membership-based network for independent mental health professionals. When a provider joins as a member practice, we empower them with the tools they need to succeed - lead generation, client matching, telemedicine software, training - basically a practice-in-a-box. We work with insurance companies for our members so that they don’t have to deal with them.
We really exist to simplify access to affordable mental healthcare, and we do that primarily by making the lives of providers as easy as possible. For example, we started with Alma co-practicing spaces, enabling providers to see patients in-person (though coronavirus quickly moved us into a predominately virtual model).
On the consumer side, we’ve designed Alma to uniquely meet the mental health needs in the market. First off, our providers are vetted. When a patient books through Alma, they know our providers have gone through a verification process, and usually their services are in-network. Secondly, consumers have the ability to find providers that match what they’re looking for, with filters for criteria such as language, ethnicity, and area of focus. Finally, we’re unique in that we provide free matching services - we commit to help patients find the right provider for their needs.
We also play a role in serving payers. Insurance companies have heard from employers that a high-quality outpatient network that has consistent availability is crucial. We help solve this by providing access to a reliable network, and by supporting our clinicians with technology, education, and better data to ensure their care is top-notch. And because payers know behavioral health must be a part of delivering value-based care in the long-run, we serve as a trusted partner that can go all the way and integrate with their ecosystem in terms of risk sharing and data sharing.
How do you make money?
My philosophy is that the best business models are those that derive value form creating efficiences. Instead of just increasing gross spend in the health system, we try to help collapse gross spend for the system as a whole and take a piece of what we help our customers save.
With that in mind, consumers don’t pay anything - our matching services are free to them.
For our providers, we charge a membership fee, but it’s a fraction of the cost of what they’ve been spending to operate.
For payers, we look the same to them as individual clincians do, but we just make it much easier to work with us. We make it easier to get network adequacy, help with functions that are difficult for payers (such as credentialing or network management), and are overall just simple to partner with as a technology company that has the software and support infrastructure to aid in day-to-day operations.
You announced a $28M Series B back in February. Can you talk about your venture journey and relationship with investors?
Yep - our most recent raise was our Series B in the beginning of February, which was led by Insight Partners. Altogether we’ve raised a total of $40.5M from a great group of investors - Tusk Ventures, First Round, Primary Venture Partners, Sound Ventures, Insight Partners, Optum Ventures, BoxGroup, Rainfall Ventures, and __able.
Now that we’re at this point with our Series B, we’ve demonstrated product-market fit and the ability to start scaling it smartly. We feel incredibly lucky to have Insight on board now - there’s nobody better at figuring out how to scale. Our investors have been particularly helpful in working through team growth and market growth - we’re hiring like crazy right now and exploring markets at a national scale so that we can serve patients wherever they are.
Where do you see mental healthcare going in the next 5-10 years?
The first thing I expect to shift dramatically is how we effectively measure quality in behavioral health. We’re starting from an okay baseline, but we have a lot further to go. As far as validated clinical assessments go, we’re really still at the beginning.
Secondly, and more conceptually, we’re just starting to shift from thinking of behavioral health as preventive rather than curative. We still orient toward thinking of mental illness, and then discuss mental health as a response to mental illness. I think we’ll see a lot of movement toward a preventive system - more preventive screenings, perhaps with primary behavioral providers becoming the norm, and a similar shift occuring in the education system. Medical school often lags a little bit behind what’s happening in the field and what people are expecting or requesting. Mindfulness, grit, and resilience are slowly finding their way into the nomenclature.
I think companies like Headspace and Calm have played a really interesting role in chanigng the tone of how we think about mental wellbeing. There are also a lot of interesting approaches focusing on specific markets or needs, such as businesses going deeper into things like ketamine or adolescent care, which I think we’ll see more of.
If you’re interested in what Alma’s up to, you can subscribe to their bi-weekly newsletter The Digest, which covers news, essays, and research on mental healthcare. If you’re looking for your next role, you can check out open positions on Alma’s job board (currently, they’re seeking a mix of community, finance, marketing, and product/engineering roles).
🩺 Clinical Coverage
Discussion of clinical concepts, studies, or perspectives on mental health and wellbeing.
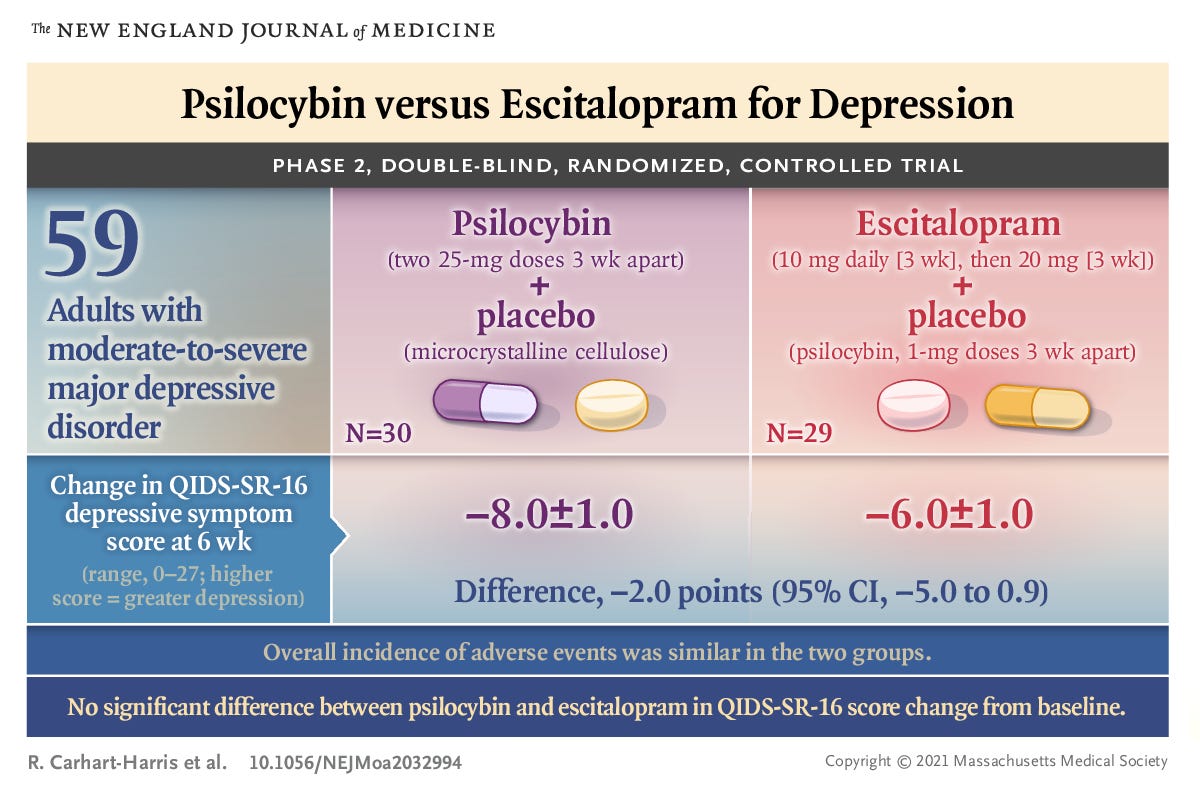
This past week, a highly-anticipated trial was released comparing the efficacy of Psilocybin versus a popular selective serotonin reuptake inhibitor (SSRI), Escitalopram, in treating depression.
Published in The New England Journal of Medicine, the phase 2, double-blind, randomized, controlled trial evaluated treatment efficacy across a patient panel of 59 participants.
The outcome? The trial did not show a significant difference in antidepressant effects between Psilocybin and Escitalopram.
What does it mean for psychedelic therapy, specifically psilocybin? Despite the outcomes remaining similar across both treatments, it’s worth noting that the Psilocybin treatment required just two doses three weeks apart, while Escitalopram was provided daily across the six weeks. Psilocybin also outperformed in several secondary measures detailed in the trial.
There is significance alone in the trial being published in such a prestigious journal, as it brings additional attention to Psilocybin’s therapeutic potential. Still, given the small sample size, additional trials with larger panels and longer durations will need to be conducted to continue comparing Psilocybin against established treatments.
💰 Recent Investments and IPOs
Rundown of recent investment news in mental health and wellness companies.
Better Therapeutics, a nutritional cognitive behavioral therapy digital therapeutics company, announced plans to go public by merging with SPAC Mountain Crest Acquisition Corp II (Link)
Real, a mental wellbeing membership company, raised a $10M Series A led by Lightspeed Venture Partners, with participation from Forerunner Ventures, Female Founders Fund, BBG Ventures, G9 Ventures, and SoGal (Link)
Scribe Therapeutics, a platform designed to help develop new therapeutics based on CRISPR, raised a $100M Series B to advance its pipeline of therapies for neurodegenerative diseases. The round was led by Avoro Ventures, Avoro Capital Advisors, OrbiMed Advisors, and a16z; they were joined by Perceptive Advisors, T. Rowe Price Associates, Wellington Management, RA Capital Management, Menlo Ventures, and an undisclosed global investment firm (Link)
StimScience, an electroceuticals company that develops brain stimulation systems, raised a $6M Seed round led by Khosla Ventures (Link)
📖 Interesting Reads
Sometimes mental health-related. Sometimes just things I find interesting.
Behind the scenes of remote therapy. The New Yorker
Beauty filters are distorting perceptions and expectations. Technology Review
The richest billionaire in every U.S. state. Forbes
Evidence suggests that muon particles are sensitive to a force that contradicts the Standard Model of the universe. NYTimes
The Winklevoss twins make a comeback. Forbes
Get out of your geographic music bubble. The Pudding
When mindfulness comes at a cost. Harvard Business Review
Tiger Global’s approach to venture. Everett Randle
Are you languishing? NYTimes
Alexei Navalny continues his hunger strike from prison. NBC News
How people get rich now. Paul Graham
Which countries are open to Americans right now? Travel and Leisure
🧠 Mindfulness Tip of the Week
Tips to improve your mental health and wellbeing.
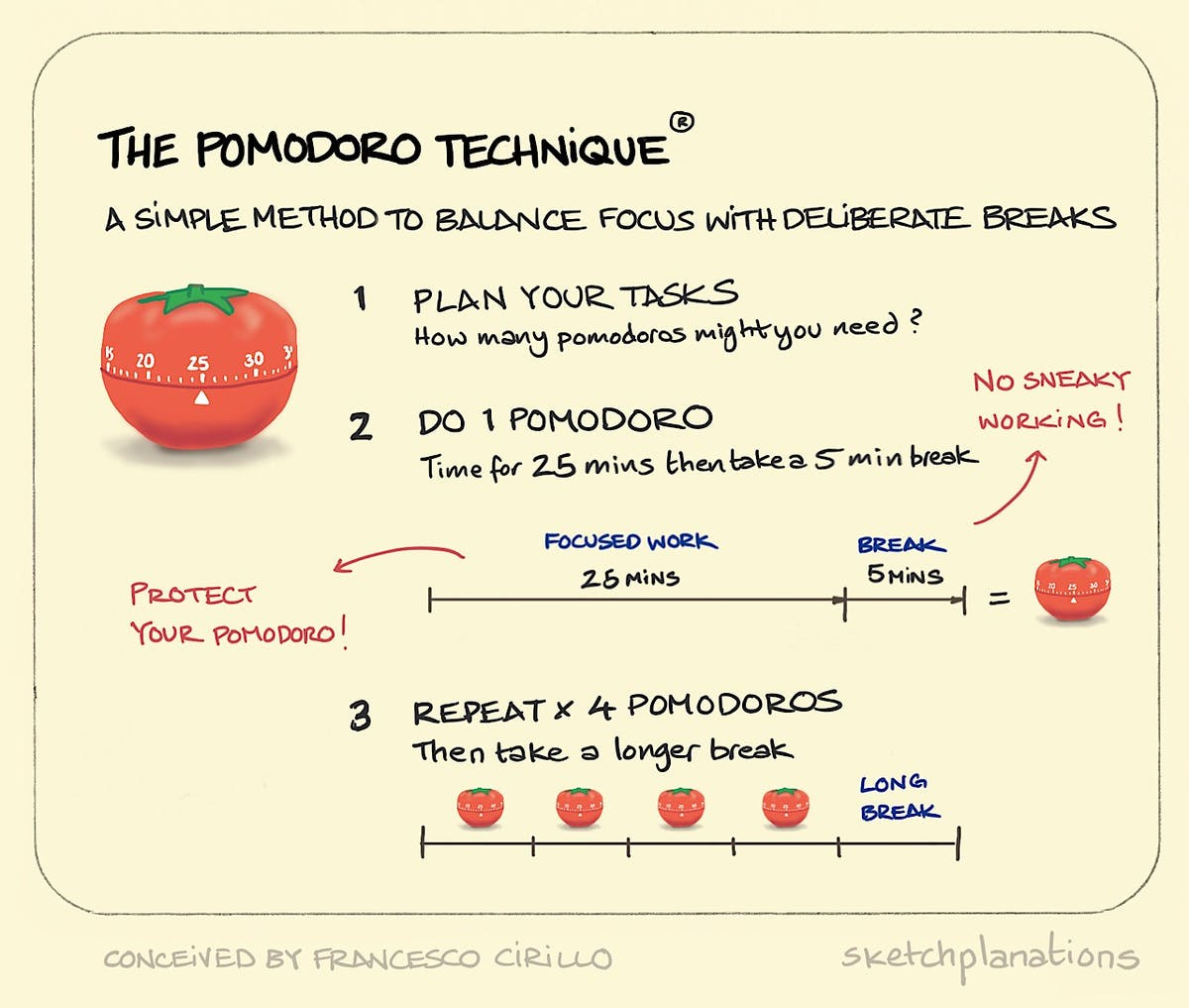
Today I figured I’d lay out a tool I’ve incorporated in the past that I’ve recently brought back into my workflow: the Pomodoro Technique.
It’s not a novel idea, and the psychology behind it is quite straightforward. Create space in your mind for dedicated work time in short bursts, and reward yourself accordingly with protected breaks.
Instead of the notorious red tomato-shaped timer, I use the Otto app, a Google Chrome plug-in. With Otto, you can apply the Pomodoro Technique to your workflow and view simple reports with insights that can help you allocate your time more appropriately.
So far, incorporating work sprints with brief breaks has helped, but the jury’s still out on whether I change my broader use of time based on the reports. I’m not sure if understanding how I’m spending my time is enough motivation to make meaningful changes…but it can’t hurt.
On Your Mind
I’d love your feedback - feel free to email me at tarockoff@berkeley.edu.
If you’re working on something in mental health and wellness, let’s talk. You can book some time with me here.
Know someone who’d enjoy On The Mind?
Was this newsletter forwarded to you?
Written by Daniel Tarockoff, an MBA student at UC Berkeley and former healthcare strategy consultant exploring the future of mental health. Born in Michigan. Based in Berkeley, CA.